PART 1: ROTATOR CUFF INJURIES
In the First Part of the Shoulder Series, we discuss the pain and problems associated with Rotator Cuff Injuries. Through this article, you will identify characteristics associated with Rotator Cuff Injuries from tendinitis, tendinosis, and strains/tears.
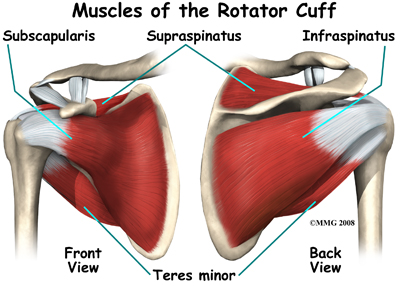
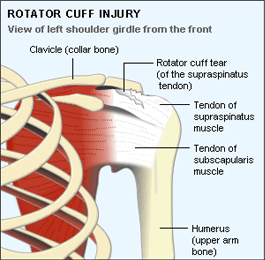
The Rotator Cuff is collectively made up a group of tendons that surround the shoulder joint to aid in stability. The four tendons have specific functions in helping with movement as well. Collectively the tendons form a “cuff” and secure the shoulder joint (glenohumeral) in place. The four tendons are formed from the following muscles:
- Supraspinatus (elevates arm)
- Infraspinatus (internally rotates)
- Teres Minor (externally rotates)
- Subscapularis (externally rotates)
While the function of the rotator cuff muscles seems simple, their role in shoulder stability and good health is much greater than simply prime movers in single path directions. These muscles, in conjunction with other areas of the upper extremity, participate in co-contraction processes to firmly secure the shoulder to promote joint centration.
Joint centration is important and is defined as the optimally placed position in which a joint is positioned during static and dynamic states. While at rest or while in motion, the orientation of the shoulder joint is required it to be optimally positioned to allow maximal weight bearing properties with uninterrupted motion reflecting range of motion and quality of the movement.
All types of injuries can affect shoulder motion, function and produce symptoms. The limitations and manner in which these characteristics display is crucial in identifying the correct disorder. In this article, we will focus on the symptoms and presentation associated with true Rotator Cuff Injuries.
Rotator Cuff injuries can range from mild to severe cases demonstrating inflammation, tendinitis, tendinosis, mild, moderate, or complete tears.
As we mentioned the Rotator Cuff is made up of tendons; therefore, this is a tendon injury. The extent of the tendon injury can vary; but due to the nature of the physiological make up of tendons, it’s response is the same—SLOW TO CHANGE….
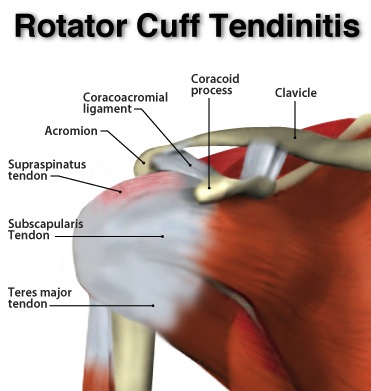
TENDINITIS
Tendinitis is inflammation of the tendon. Specifically, in this case, the inflammation of the rotator cuff tendons; which of the 4 tendons? That will reveal itself in an examination and history presentation. The inflammatory response of the tendon can occur for various reasons, the more common is immediate injury, overuse and excessive repetition of overhead activities; individuals like baseball players, swimmers, tennis players, golfers, volleyball players, football players, weight lifters, or mundane factory workers with repetitive tasks. These individuals are prone to inflammatory disorders if the shoulder is improperly moved or the movement is frequently overused in one direction repeatedly without stretching our moving in other directions.
In many cases, the inflammatory response is simple to alleviate. This stage will require rest, reduction in activity, anti-inflammatories, and maybe some ice. For more advanced cases of rotator cuff tendinitis, a cortisone injection may be recommended.
The reason why you produced inflammation is the underlying issue; addressing poor biomechanics, tight tissues, lack of mobility, loss of range of motion, or compensation of the shoulder mechanics. These reasons can affect the shoulder and produce irritation which in turn lead to inflammatory conditions.
PAIN PRESENTATION
- Localized Pain (Pain does not travel; ALWAYS stays in one area)
- Constant Pain (Every hour, minute, second; during activity and rest)
- Increased Use of Shoulder Increases Pain
- Decreased Use of Shoulder Decreases Pain
- Acute Time Frame
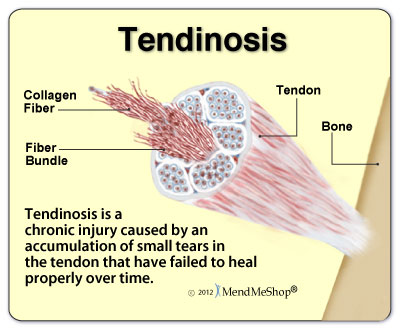
TENDINOSIS
Tendinosis is internal tendon degeneration; it is a stage of imbalanced tendon repair and tendon degeneration. The same subgroups of overhead dominant individuals are a risk for tendinosis. The amount of degeneration can vary in these cases being affected by age, weakness, tissue pliability, mobility, and nutritional aspects.
Tendinosis can be a chronic problem if the scar formation during the repair process of the degenerative tendon is not remodeled appropriately. When injured, the tendon does not heal by growing more tendon-like properties; rather, it repairs by laying down scar tissue-like properties. Therefore, a weaker property make up than the original tendon tissue. While this sounds disheartening, the scar tissue yet remains sufficient and strong enough to provide function to the shoulder and live pain free if the degeneration is not irreparable. The key to remodeling the scar tissue during the repair process of the degeneration is to determine the directions in which to begin moving the shoulder and add a resistance to invoke an adaptive response. Remodeling the scar tissue will produce a symptom of pain or discomfort during the therapeutic exercise. Upon release of the resistance, the symptom of pain or discomfort should be abolished. This response is a necessary response in remodeling scar tissue.
PAIN PRESENTATION
- Localized Pain (Pain does not travel; ALWAYS stays in one area)
- Intermittent Pain (Pain comes & goes)
- Increased Use of Shoulder has No Effect on Pain
- Decreased Use of Shoulder has No Effect on Pain
- Specific Directions of Shoulder Movement Produce Symptoms (While some directions do not provoke symptoms)
- Chronic Problem (>12 weeks)
TEARS / STRAINS
The word strain and tear are synonymous. These terms are used interchangeably, but the more detailed expression of these terms is defined based on the severity of the tear. A strain is damage to the muscle or tendon that is elongated with great force to cause structural damage to the muscle fiber. The tears are categorized by grade level.
- GRADE I: overstretched tendon, or mild tear with little or no instability of the joint
- GRADE II: greater tear, incomplete tear, moderate instability of the joint
- GRADE III: completely ruptured, torn; complete tear; significant instability of joint
With rotator cuff tears / strains, the treatment varies depending on the person’s shoulder. According to the Journal of Bone & Joint Surgery, Factors Affecting Rotator Cuff Healing, the recovery will be dependent on the size of the tear, atrophy of muscle, fatty infiltration, and bony spurs. While other factors play into account such as age, tissue health, and mental willingness to improve; the main focus is identifying the correct treatment. Typically, Grade I tears do not require surgery; Grade II tears may or may not require surgery; and Grade III tears always require surgery.
The rehab process that comes with Grade I tears is progressive; initially focusing on single plane movements insuring remodeling of the scar tissue that is laid down to close the tear; followed by loading strategies and corrective movement exercises to influence proper joint centration & biomechanics.
Grade II rehab will take longer than Grade I, but very effective given patient dedication and appropriate treatment plans. The similar treatment presentation as mentioned above, except the rehab process of single plane directions may be multiple directions. The continuance of adding an increasing load to elicit adaptive tissue response is necessary for the repair process.
Grade III tears will require surgery. Post-Surgery Rehab requires progressive multi-plan movement; initially, one direction is used, followed by multiple directions rather quickly. The common theme is increasing the range of motion and gathering strength by loading exercises. The loading exercises provide strength in stability to ensure proper ability to withstand dynamic movement. Correcting any compensations or improper biomechanics is necessary to avoid re-straining the rotator cuff tendon.
PAIN PRESENTATION
- Intermittent Pain
- Localized Pain
- Specific Directions of Shoulder Movement Produces Pain
- Feelings of Weakness
- Decreased Range of Motion
- Acute, Sub-Acute, Chronic Time Frame
If you or someone you know struggle with include Rotator Cuff Problems/Pain, please give us a call. We help people who suffer from all types of physical injuries.
We are Dedicated to Get You Better Through Movement…
For Appointments Call (219)-310-8822
Dr. Artemio Del Real DC, Cert. MDT, CSCS